
UNDERSTANDING HAIR LOSS
Share
BEFORE WE BEGIN...
The information provided in this article is for information purposes only and should not be considered as a substitute for medical advice. Please read our disclaimer at the bottom of this page for more information.
Medically Reviewed by Professor V. Jolliffe
INTRODUCTION
If there is one certainty when discussing hair loss it is that it can affect anyone, irrespective of age, ethnicity or sex, and it is much more common than you may think.
The causes and reasons for hair loss are incredibly varied and for those of us suffering from losing our locks, it can be very challenging to wade through the quantity of sometimes confusing information online to find out exactly what’s going on. Don’t worry, we are here to help you understand the commonest reasons why we lose our hair.
It's helpful first to look at the hair cycle and understand the fascinating and complex journey your hair takes.
Whether hair thinning is a new problem for you, or one which has been a nuisance for a while, we'll discuss some of the most common causes of hair loss and how they can be managed.
THE CAUSES OF HAIR LOSS
The most common causes for hair loss broadly fall into 3 categories; thinning related to sensitivity to androgens (often genetic), shedding related to a number of medical conditions including medications, stress and anxiety, and damage related to styling practices.
Let's have a look at each of these causes in turn, starting with one of the commonest causes- sensitivity of androgens. This is known as Androgenetic Alopecia or Pattern Hair Loss (the two are the same condition) and whilst it is easily recognised in men, it can affect women too.
1. ANDROGENETIC ALOPECIA/PATTERN HAIR LOSS
This type of loss is estimated to affect about 50% of men over the age of 50, and about 50% of women over the age of 65 accordingly to the British Association of Hair Restoration Surgery (BAHRS) who point out that those suffering from Androgenetic Alopecia may be inheriting hair follicles with a genetic sensitivity to Dihydrotestosterone (DHT) which is derived from testosterone.
While many men start losing their hair around the hairline and crown (resulting in a receding hairline and a bald patch), female pattern loss tends to start with widening of the part width and reduction in hair density over the crown, as the individual hair fibers become thinner and shorter in this area. The genetics of pattern loss are not fully understood, but are probably more relevant in male pattern loss than female pattern loss. Female pattern loss may be associated with conditions which increase circulating androgen levels or are associated with increased sensitivity to circulating androgens such as Polycystic Ovary Syndrome.
When discussing Pattern Hair Loss, doctors may often refer to one of the universal classification systems - The Norwood Scale (for men) or the Ludwig Scale (for women). Let’s look at what these are and how they help classify the degree of your hair loss;
- THE NORWOOD SCALE
The Hamilton-Norwood scale, more commonly known as the Norwood Scale, was first introduced in the 1950s by Dr Hamilton but later updated in the 1970s by Dr Norwood and is perhaps the most commonly used classification system for male pattern hair loss.
This scale is a helpful visual aid to understand what stage your hair loss may be at and also be useful to determine the types of treatments that may be more beneficial for you at each stage of the scale.
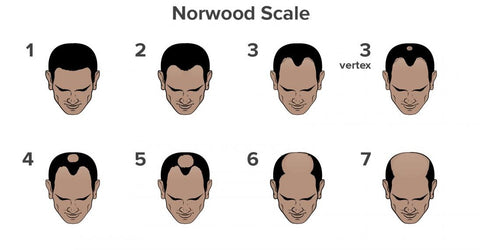
This first stage in the Norwood scale is where you would be considered as having a full head of hair, with little to no visible signs of hair loss or receding hairline.
At stage 2, you would be considered to be showing slight evidence of your hair receding but this would be regarded as barely noticeable.
STAGE 3
By stage 3, your hair loss is generally more noticeable and you typically see the hairline receding from the temple area giving the classic “M” shape to your hair.
As above, this sub-classification also incorporates hair loss from the crown
STAGE 4
Stage 4 on the Norwood scale would be determined as significantly noticeable. At this stage, it would be apparent that you are experiencing hair loss
STAGE 5
By stage 5, there is likely to still be some hair covering the scalp but the hair continues to recede from the sides.
STAGE 6
With far more skin visible on the scalp at stage 6, by now you are likely to have hair remaining on your sides but the crown and hairline have joined across the scalp.
STAGE 7
In the final stage on the Norwood scale, at stage 7 there is little to no hair on the scalp. While hair remains at the side and back, any hair grown on the top would like to be very weak and thin.
In addition to the 7 primary stages, there are also 4 class A patterns found in stages 2 through 5. These are less common but signify a more aggressive loss from the front of the hairline (ref: Bernstein Medical).
- THE LUDWIG SCALE
Designed in 1977 by Dr. Ludwig as a method of classifying female pattern hair loss according to a scale of severity, this scale is designed to classify the extent of the condition and assist in deciding the best course of treatment,.
There are a number of other scales used by doctors such as the Sinclair, Savin and Olsen Scale, but let's have a look at the Ludwig scale.

GRADE 1
Grade 1 on the Ludwig scale is typically identified as minimal thinning. At this stage, hair loss at this stage may go unnoticed by other people but appear and feel generally thinner to you.
GRADE 2
At grade 2, this could be considered more moderate hair loss. By this stage, you may notice a widening at the parting of your hair and a more moderate reduction in the thickness of your hair along with an increase in shedding.
GRADE 3
Often described as diffuse thinning, this type of hair loss creates a see-through appearance on the top of the scalp. This is the rarest, most severe type of hair loss for women and it’s less easy to disguise with hairstyling techniques.
2. HAIR SHEDDING RELATED TO MEDICAL CONDITIONS ( EFFLUVIUM)
This is also a common cause of hair thinning especially in women. The hair cycle is extremely sensitive to changes in its micro-environment which can result in shortening of the active growth phase of the cycle ( Anagen) and early entry into the shedding part of the cycle (Telogen). This results in increased hair loss and may in some cases reveal an underlying pattern loss. The commonest reasons why this process may occur include post pregnancy, thyroid disease or anaemia, poor scalp health, certain medications and stress and anxiety. Unlike pattern hair loss when, without treatment, the hair fiber gradually gets shorter and thinner over time, in telogen effluvium the fibers themselves can normalise once the underlying condition causing the effluvium has been treated or resolved.
ANAEMIA
Anaemia occurs when there is a deficiency of either iron or Vitamin B12 which leads to inadequate number of or performance of red blood cells.. It may be asymptomatic but can also result in tiredness and shortness of breath. Whilst there is some controversy about its role in hair health, most dermatologists who treat patients with hair loss would agree that low iron stores can be associated with poor hair growth and shedding.
HYPOTHYROIDISM / HYPERTHYROIDISM
Under- or -over active thyroid and indeed sometimes the medication used to normalise thyroid levels can all be associated with hair thinning and shedding. Furthermore, sometimes disorders of the thyroid may be caused by autoimmune disease, which can also in itself affect the hair follicle.
DANDRUFF AND SCALP PSORIASIS
Skin conditions on the scalp can commonly cause hair loss, including dandruff seborrheic dermatitis and scalp psoriasis. Both cause itchy, inflamed skin on the scalp that can lead to intense and prolonged scratching. This scratching can damage the hair follicle and cause breakage to the strands, resulting in increased fall out. The inflammation itself resulting from dandruff also impacts negatively on hair growth and fiber quality.
STRESS
In clinical practice stress is a very common reason for hair loss,. Extreme and prolonged stress can cause an increase in the production of adrenaline and cortisol which can slow hair growth at the hair follicle level but also may raise testosterone levels.
WEIGHT LOSS/DIETARY CAUSES
Rapid weight loss and restrictive/crash dieting can be an unexpected cause of hair loss and is a cause we commonly see in clinics. Vegetarian and vegan diets may sometimes lead to low iron or inadequate protein intake and it is important in these circumstances to consume protein rich foods such as quinoa, lentils, black beans and Chia seeds.
PREGNANCY
Whilst not a ‘medical’ condition this is one of the most common causes of hair loss amongst new mothers, postpartum alopecia generally occurs a few months after giving birth, When pregnant, the increased oestrogen produced prolongs the growth phase of the hair cycles (anagen) giving longer thicker hair. With delivery and the drop in oestrogens, the hair cycle enters telogen and shedding occurs.
CHEMOTHERAPY
Some cancer treatments such as certain types of chemotherapy or localised radiotherapy can result in hair loss. Fortunately in most cases hair regrows after completing chemotherapy, although it is not unusual for the texture to change and occasionally scarring hair loss can occur. Support is available both from the cancer multidisciplinary teams and charities such as Look Good Feel Better (LGFB) which can provide support and advice on wigs, along with skincare and make-up workshops.
3. STYLING RELATED HAIR LOSS
TRACTION ALOPECIA
Traction alopecia occurs as a result of tension put onto the hair follicles over time, for example overuse of extensions, weaves, tight ponytails, and braids. Any style which pulls the hair can damage the root which can in certain circumstances lead to scarring and permanent hair loss.
TRICHORRHEXIS NODOSA
This is the name given to localised areas of damage along the hair fiber which have become weakened by styling such as excess heat or traction or straightening. The hair becomes very fragile at these sites and as a result snaps, leading to hair which cannot grow long and looks thinner particularly near the end of the fiber.
Whilst we have discussed the 3 commonest causes of hair loss there are a number of other less common causes including alopecia areata or autoimmune hair loss.
ALOPECIA AREATA
Alopecia Areata is an unusual cause of hair loss which typically starts with one or more small, smooth patches appearing. The condition is an autoimmune disorder, where the body triggers an autoimmune attack on the growing follicle.
Alopecia Areata can begin at any age and affects both sexes.
Although no one is quite sure what causes these triggers, fortunately the hair can regrow even after months of extensive hair loss and for most sufferers hair loss is limited to patches. Rarely it can become more extensive and affects brows, lashes or body hair.
FURTHER READING
Why not check out our other articles;
CONCLUSION
Although this is not an exhaustive list, this hopefully helps to show you that there are many causes of both long-term and temporary hair loss. As hair loss is such a complicated subject, it is important to take the time to speak to a medical professional to understand what may be causing your own loss before looking at any potential treatment options.
DISCLAIMER
While our aim is to provide you with up-to-date and relevant information, drugs affect each person differently. As such we cannot guarantee that this information includes all possible side effects and this information is not a substitute for medical advice. Always discuss treatment options and possible side effects with a healthcare professional who knows your specific medical history.




